Flight #23 - Aeromedical Safety - The Risk Matrix
Welcome to The Flight Shrink newsletter! This is Dr. Kevin Heacock.
A little housekeeping before I get started today. Last week I used “previous suicide attempt” as a mental health concern to discuss the 1% rule. Unfortunately, I neglected to provide resources for those struggling with suicidal thoughts. Since the first Flight Shrink newsletter and podcast I have listed resources at the bottom of every Email and in the show notes of every podcast episode. But in case you haven’t seen those, if you or someone you know needs help, please visit 988lifeline.org or call or text the Suicide & Crisis Lifeline at 988.
I talked some last time about my experience at the NTSB Aviation Safety Summit on Navigating Mental Health in Aviation. If you’d like to read more about the NTSB meeting, The Washington Post does a good job covering it in an article this week.
I have seen people saying this article points out the harm current policies have caused to pilots. At the same time I wonder how many lives, including the lives of pilots, such policies may have saved. Unfortunately, there is no way to capture how many accidents were avoided because some pilots were not allowed to fly due to an unsafe medical condition. Hopefully there is a solution that allows pilots to get the care they need while maintaining a safe airspace for everyone. One possibility could be a risk matrix as I have alluded to in the last few posts and will discuss today.
In previous posts I’ve talked about the 1% rule which was the traditional way of thinking about aeromedical safety. The 1% rule being that if there is a 1% chance that within the next year a pilot’s medical condition could lead to a catastrophic failure of a flight, the risk is too high to allow that pilot to fly.
But as Dr. Giovanetti said at the NTSB meeting, the FAA uses a method that considers the chance of a medical event occurring along with the severity of the event, should it occur. She didn’t say they use a risk matrix, but that is essentially what a risk matrix is. But a little more goes into understanding and using a risk matrix.
For the most detailed explanation of the current understanding of a risk matrix I would point you to the USAFSAM Aeromedical Consultation Service Medical Risk Assessment and Airworthiness Matrix paper in the July 2023 edition of the Aerospace Medicine and Human Performance journal, sometimes referred to as The Blue Journal. Full disclosure, while I was not an author on this paper, I was involved as one of the specialists who helped validate the risk matrix. While the paper gives a much better and fuller explanation, I will try to explain it as best I can in basic terms and show how it might be used to think through a diagnosis like Major Depressive Disorder.
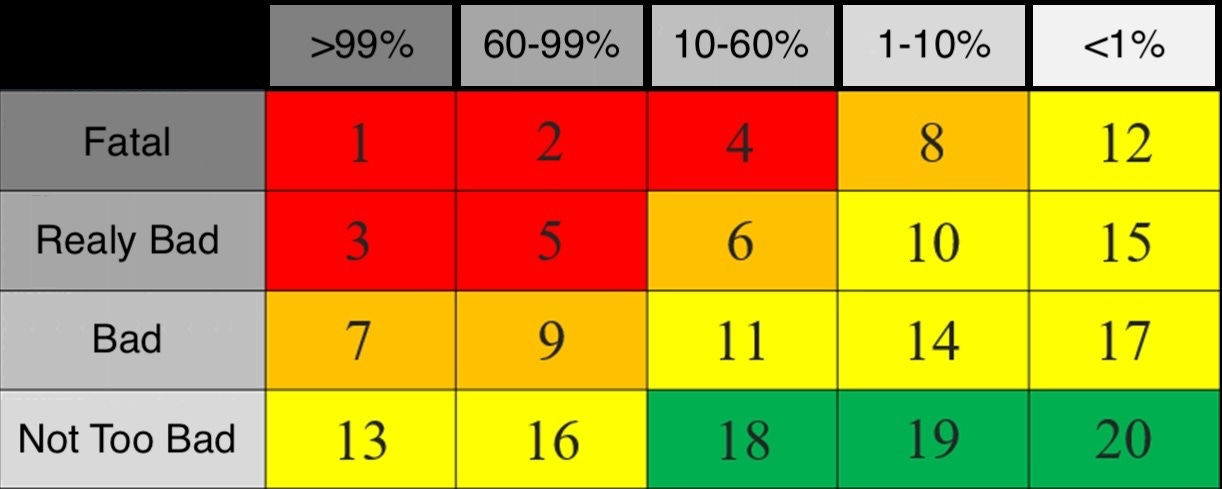
Here is a risk matrix that shows percentages across the top. The percentages at the top are the probability of a medical event occurring within the next year. So something like a seizure, which as was discussed in the last two posts has a 36% chance of occurring in the next year, would be in the middle column of 10-60%.
The severities are seen along the side and are as follows:
Fatal event would be something like a plane crash in which someone in the plane or on the ground dies
Really Bad event would be like the plane crash landing in a way that causes significant injuries, but no one dies
Bad event would be like something that causes an inflight emergency that requires immediate landing, but no significant injuries
Not Too Bad event would be like a medical event that doesn’t cause any changes to the flight, but needs to be taken care of as soon as they land
The intersection of the 5 probability ranges across the top and the 4 severities along the side lead to 20 boxes numbered 1 through 20 with the most risk being attributed to box 1 as it has an almost 100% chance of occurring and if it did it would be fatal. And then the numbers are color coded with 1 through 5 being red indicating a high risk, 6 through 9 are orange indicating a serious risk, 10 though 17 are yellow, a medium risk, and 18 through 20 are green, a low risk.
Now that you’re oriented to the risk matrix, it’s helpful to know where these ranges of probabilities came from and why some combinations of high probability and high severity are deemed high risk, while other combinations are only a medium risk.
This aeromedical risk matrix is based on the concept of airworthiness. Airworthiness is the suitability of an aircraft for safe flight. And this applies not just to the aircraft, but also to the pilots who operate it. With this understanding that airworthiness is no different between how the plane functions and how the pilots function, the same parameters of risk acceptance can be applied to the pilots as are applied to the plane itself.
Again, I would point you to the paper in The Blue Journal to see how the probabilities of a plane failing were calculated into the probability of a medical event occurring. The math is there and it works, but I struggle to understand it, let alone explain it. But just know that the same probabilities of concern for aircraft failure are matched to the probabilities of medical events to give us the columns in the matrix. Similarly, the severities are equivalent whether an aircraft fails leading to a fatal accident or the pilot has a medical event.
And then the colors indicating the significance of the risk come from this same airworthiness concept. If a plane has a 30% probability of failing in the next year, and its failure would cause a fatal accident, then that is a 4 in the matrix, which is a red box indicating a high risk. And if a plane has less than a 1% chance of failing, even if it would result in a fatal accident, it is only considered a medium risk in a yellow box because that corresponds to box 12.
Remember the 1% rule? If there is a 1% chance that within the next year an event would lead to a catastrophic failure of a flight, the risk is too high? Well that’s box 12 in the risk matrix. That is the traditional way of thinking about things. You can see that if it’s higher than 1% it moves into the next column to the left, and if it were fatal it would fall in box 8 which is orange indicating a serious risk. So the 1% rule still matters if the medical condition were to lead to a fatal outcome.
But what the matrix does, is it gives the stakeholders an ability to see what the risk really is. And they can decide, if it is something they’re willing to take a high or serious risk on. Or they can continue to play it safe and not accept anything above a medium risk as the 1% rule has traditionally done.
The matrix also gives the stakeholders an opportunity to consider certain events differently based on the severity of the outcome should it occur. So while they may never accept the high risk of a seizure that has a 36% chance of occurring because it could be Fatal, maybe would accept the risk of someone with a 30% chance of having low back pain in the next year as the outcome would only be Bad in severity and so would be an 11 in the risk matrix corresponding to a medium risk.
The risk matrix also gives the stakeholders the opportunity to adjust their risk tolerance based on the availability of resources and other variables. For instance, if there was an endless supply of pilots, maybe only green low risks would be accepted. But if there was a significant shortage of pilots, maybe the stakeholders would accept more yellow medium and maybe even orange serious risks.
And finally, seeing the risk in this way, the risk can be adjusted based on the ability to mitigate the probability or severity of the event. Take a pilot with significant sleep apnea to the point they get such poor sleep at night that they’re tired all day. And so it is very likely they could fall asleep while flying and cause a fatal accident putting them at high risk, at least in red box 4. However, if they get gold standard treatment like CPAP, a mask they wear at night that keeps their airway open throughout the night, and they regularly get good quality sleep, the chance they will fall asleep during the day is now less than 1% putting them at medium risk in yellow box 12.
Likewise, the severity of the outcome could be reduced were the medical event to occur by making sure a pilot flies with another qualified pilot. So while someone with significant headaches, where the future recurrence rate is imprecisely-predictable, might not be safe to fly alone, if they were restricted to only flying when they are with another qualified pilot, the severity, rather than being Fatal or Really Bad were they to crash because of their headache, would be reduced to just Bad because the other pilot could land immediately. And this would lead to a reduction in the aeromedical risk that most stakeholders would probably deem acceptable.
Just saying all that seems really complicated to me. I’ve had to go over this several times to make sure I’m understanding it correctly. So if you need to maybe go back and listen or read again and follow along with the risk matrix in the newsletter, please do.
To try to summarize it though, the risk matrix is based on already established and accepted risk tolerances for aircraft, based on the probability of an event and the severity of the outcome should the event occur. Applying it aeromedically uses the same probability and severity categories and risk stratifies medical events pilots may be susceptible to given the quality of their health.
Perhaps a better way to understand it is to go through a diagnosis and put the risk matrix through its paces. So let’s take Major Depressive Disorder as our example.
In the United States the risk for anyone having a Major Depressive Episode is 10.4% per year. And in 2016 a Harvard paper found that 12.6% of pilots met criteria for a Major Depressive Disorder. Now this is kind of interesting because if you look at the matrix this puts everyone, including pilots, in the middle column. And if you think Major Depression, with its poor sleep, low interest, guilt and worthlessness, low energy, poor concentration, appetite problems, slow reactions, and suicidality, could lead to a Fatal or Really Bad outcome then you’re already looking at a high or serious risk in red box 4 or orange box 6.
So surely untreated depression that rises to the level of a diagnosable condition is a significant risk to flying. But every individual is different. And a risk matrix like this is usually used once someone has been identified as having a Major Depressive Disorder and has gotten treatment and is presumably doing better. So it is probably better used to look at the probability of a recurrence of a Major Depressive Disorder in someone who has already had one.
In that case, one study shows 39% of those who had an episode of Major Depressive Disorder had a recurrence within the first year. So that still keeps us in that middle column. And either treatment to reduce the probability of recurrence would be needed or some way of mitigating the severity would be needed should the depressive symptoms recur and cause difficulty for a depressed pilot to function.
Of note, once someone has had a second episode of Major Depression, the risk of future Major Depressive Episodes just keeps going up. If they’ve had two depressive episodes there is a 70% risk of a third episode, and if they have a third episode there is a 90% risk of a 4th episode. You can see that would move them over into the next column to the left indicating an even higher risk. So the more episodes of depression a pilot has in their life, the higher the aeromedical risk.
But going back to someone who has had just one Major Depressive Episode, you might think that treating them would be a significant mitigator, but really, all of the studies that look at recurrence rates are done with patients who are in treatment. Because obviously it would be unethical to let people suffer through depression in a study and not provide treatment. So even with treatment it’s not clear how much the probability of recurrence can be reduced. But surely it is being reduced some, but how much? And it’s probably different in each person depending on what treatment they’ve had and how they responded to it.
So then it becomes an individual case-by-case evaluation to determine if each pilot’s specific treatment has improved their symptoms and decreased the probability of recurrence to move them far enough to the right on the risk matrix to reduce the aeromedical risk enough to consider them safe to fly.
Again, I feel like this is pretty complicated and hard to explain. I’m not sure I’m doing a great job of it either. But hopefully you can at least see how it’s not so cut and dry as to say, “sure a pilot had some depression in the past, but they’re not depressed now, so what’s the big deal, let them fly.” Because the aeromedical risk isn’t based on how they are doing right now, but on the probability of their impairing symptoms recurring at some point in the future.
So it really does require a look at each case individually to see how severe their depression was, what kind of treatment they had, how they responded to that treatment, and how they have done for a period of time following that treatment. And also to see how they have managed recent stressors as an indicator of how they may handle future stressors without succumbing to the same potentially impairing depressive symptoms again.
Alright, well, I think I’ll leave it at that for now. Thanks for sticking with me if you made it this far. With the next two weeks being holiday weeks, I may not post another newsletter until 2024. I was thinking I might do a look back at the first 6 months of The Flight Shrink and talk about how things have been going and what the next year might hold. But we’ll see. I may just take some time for my own self-care which for me is relaxing with family and not putting extra tasks on my plate.
I wish you all Happy Holidays and I hope you take some time for yourselves this holiday season too.
For now, thanks for logging another flight with The Flight Shrink. I hope you liked this one. If so, please like and share. And…
Keep on flyin’!
Seeking Aeromedical Guidance
The Flight Shrink newsletter and podcast is an extension of my civilian HIMS Psychiatry practice. I would be happy to consult with you confidentially on any mental health related aeromedical questions. Just email me at kevinheacockmd@flightshrink.com and for just $45 you’ll get your answer from an FAA certified AME and HIMS Psychiatrist with over 17 years of aeromedical experience.
Support The Flight Shrink:
Stay tuned to The Flight Shrink for more insights into aviation mental health. If you find The Flight Shrink valuable, I invite you to subscribe and share this post with your fellow aviators, friends, family, and colleagues. Leaving a 5-star review on Apple Podcasts or Spotify can make a big difference. And now, you can support The Flight Shrink with a one time contribution of any amount on Venmo to username @flightshrink.
I love hearing from my readers and listeners, so feel free to Email me or connect with me on social media with the handle @flightshrink.
Until next time...
I'm Dr. Kevin Heacock, The Flight Shrink... Keep on flyin’!