Flight #20 - Unapproved Antidepressants by the FAA - What Pilots Need To Know
Welcome to The Flight Shrink newsletter! This is Dr. Kevin Heacock.
Just some updates while we taxi before taking off on today’s flight. There has been a lot of talk about pilot healthcare avoidance in the last few weeks, especially pilot avoidance of mental health care given some recent events that have been in the news. I see quite a divide in how some are thinking about this topic. Some see the recent events as evidence that pilots avoid seeking mental health care, while others see them as evidence that pilots definitely should have to meet high mental health standards.
There is some level of risk that needs to be accepted when participating in the aviation business. Pilots may have one level of risk they are willing to take. Airlines may identify another level of risk as acceptable. While government agencies and the general public (passengers) may have another. But we all fly in the same national air space, and so some agreement must be made on what level of risk is acceptable. Once that risk level is agreed upon, the risk for mental health conditions like Major Depressive Disorder and Generalized Anxiety Disorder can be looked at, and so can typical stressors that cause non-diagnosable symptoms of depression and anxiety. And then the level of risk involved with these conditions can be determined to be higher or lower than the agreed upon level of acceptable risk. If the risk is lower than the accepted risk level, then a pilot can fly with that condition. But if the risk is higher, then the pilot will have to show stability for a period of time that is sufficient to mitigate that risk to an acceptable level.
I know these topics can be highly debated. The best way to talk about them seems to be sharing anecdotal stories and seeing how they line up with known data from research. Certainly more research could be done, but that doesn’t help anyone here and now. So the best we can do in the media, social media, newsletter, and podcast realm is to share our stories so people struggling with these issues know they’re not alone and that there is a way forward.
The more mental health stories we can share, the more we can reduce the stigma that keeps people from getting help. I’ve listened to some other podcasts where pilots tell their mental health stories. And, while some pilots have been frustrated with how long it takes for them to get back to flying, or in some cases, that they can’t fly anymore, none of them regret getting help and improving their mental health. All of them recommend other pilots with mental health concerns seek care. Hopefully, The Flight Shrink podcast and newsletter is helping some pilots out there manage any mental health symptoms on their own or encouraging them to see a mental health professional if needed. If you’d like to share your aviation mental health story email me at kevinheacockmd@flightshrink.com and tell me a little bit about yourself and your interests in aviation mental health.
With that said…let’s prepare for take-off on today’s flight.
Continuing with the theme of the last several flights, I will be talking about antidepressant medications and the aeromedical acceptance of those treatments. Flight #18, discussed the first four antidepressants approved by the FAA for use in pilots, the SSRIs (Selective Serotonin Reuptake Inhibitors): Prozac, Zoloft, Lexapro, and Celexa. And Flight #19 talked about the most recent addition to the FAA approved list of antidepressants, Wellbutrin. Today I’ll discuss other antidepressants that may be used in general clinical practice, but are NOT currently approved by the FAA for use in pilots.
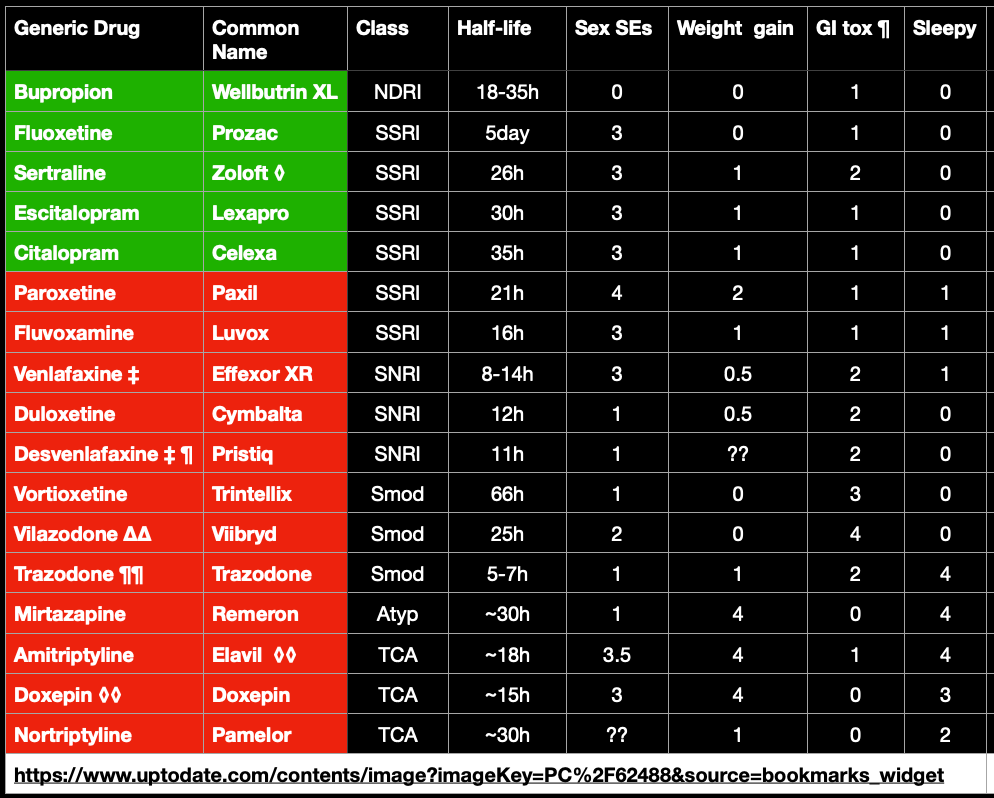
In the newsletter there is a chart of all the antidepressants I’ll be talking about along with their side effect potentials. You may want to refer back to this as I discuss these medications. The approved antidepressants are highlighted in green and the unapproved ones are in red. They’re grouped by class, but otherwise not in any particular order.
Since the 4 SSRIs were the first antidepressants approved by the FAA, I’ll start with the other SSRIs that are not approved: Paxil and Luvox. As you can see from the chart, they have a similar side effect profile as the approved SSRIs, with the addition of some potential for sleepiness. As you might imagine, a pilot taking a pill that can make them sleepy is probably not the best idea. But this is probably not the main reason they have not been approved.
To understand why these medications may not be approved, I’ve added a new column in the chart this week and it is the half-life of each drug. The half-life of a drug is the time it takes for the concentration of the drug in the body to decrease by half. So, for instance, Zoloft’s half-life is 26 hours. So if you take it first thing in the morning, when it’s time to take it again 24 hours later, the next morning, you’ve still got more than half the dose in your body. By taking it every day at the same time, a steady concentration of the medication is maintained without much fluctuation in the level you need to see the benefits.
However, you’ll note for Paxil, the half life is only 21 hours. So if you take it every morning, by the time you wake up to take it the next day more than half of it is already out of your system. This can lead to fluctuations in the level of the medication in your system. Rather than a steady concentration, you might have more ups and downs of that level. Some patients tell me they definitely notice this if they don’t take their Paxil immediately upon waking.
They may even have what patients tend to call “withdrawal” symptoms, but psychiatrists tend refer to as discontinuation effects. This can happen when the level of the medication in your system drops quickly. Common discontinuation effects include flu-like symptoms, sleep disruption, and sensory or movement disturbances. Perhaps most concerning to some of my patients are what they describe as “brain zaps” or electrical shocks going off in their head or shooting down their arms and legs. So, you can imagine if a pilot missed a dose and had any of discontinuation effects like these while trying to fly, it could be quite distracting.
Luvox, with its 16 hour half-life has the potential for similar discontinuation effects. However, Luvox is typically prescribed to be taken two times per day. As I discussed last week with Wellbutrin SR that is also prescribed to be taken twice a day, patients often forget to take the second dose, so once-a-day dosing tends to be more effective. And with all a pilot has to do while flying, having to remember to take their medication with them so they can take a second dose mid-flight leaves a lot of opportunity to miss a dose and have those concerning discontinuation effects.
After the SSRIs, the next most commonly prescribed class of antidepressants are SNRIs (Serotonin and Norepinephrine Reuptake Inhibitors). In addition to affecting the serotonin system like the SSRIs, these medications also affect the norepinephrine system and can have an effect on depression and anxiety symptoms through another neurotransmitter pathway. SNRIs have a similar side effect profile to the SSRIs, but again you’ll notice short half-lives for the three listed in the chart, Effexor XR, Cymbalta, and Pristiq.
Of the SNRIs, Effexor XR is probably the most commonly prescribed. XR here stands for extended release. I have almost never seen the immediate release version of Effexor prescribed, probably because, for similar reasons addressed above, it has to be taken two to three times a day to maintain a steady level in the body. Even Effexor XR has a relatively short half-life. Because it has some sleepiness potential some patients end up taking it at night. And so in the evenings, as bedtime approaches, some patients describe their depression and anxiety symptoms worsening or getting those discontinuation effects. This is why it is probably best to take medications like this in the morning so those dips in the level of the medication in the body can be slept through and those symptoms are not experienced.
Cymbalta is probably the next most common SNRI and has developed a reputation for also helping with chronic pain. So when someone has physical symptoms like back pain, fibromyalgia, or neuropathic pain along with their depression and anxiety, Cymbalta is often considered a way to treat all of these conditions at the same time with one pill. I have had limited success with using Cymbalta in this way in my clinical practice and find that treating depression and anxiety as fully as possible with an SSRI is often enough to manage the physical symptoms as well. And as you can imagine, if a pilot has all these physical symptoms in addition to depression or anxiety that may indicate Cymbalta as a good choice, the level of physical and mental symptoms suggesting this indication may be too much for the pilot to continue flying safely.
The newest SNRI is Pristiq. It has only been on the market for about 15 years and has been available as the generic desvenlafaxine for about 5 years. It is very similar to another SNRI, Effexor (venlafaxine), and they can both increase blood pressure and heart rate and so should have regular monitoring if used. And so perhaps you can see why Pristiq and the other SNRI antidepressants haven’t been approved for use in pilots yet.
The next category of antidepressants are the serotonin modulators (listed as Smods in the chart in the newsletter). The most commonly utilized of these is probably Trazodone. Trazodone is an older medication that used to be used to treat depression. Unfortunately, it caused a significant amount of sedation at the doses used to treat depression and had to be dosed multiple times a day. So now it is typically only used at lower doses as a sleeping pill and helps people get some sleep. But it doesn’t have much of an antidepressant effect throughout the day given its short half-life.
The FAA generally recommends waiting 5 half-lives before resuming flight duties following the ingestion of a medication that causes sedation. Five half-lives is about how long it takes for the medication to be completely out of your system. With a half-life of about 6 hours, that would mean you couldn’t fly for about 30 hours after taking Trazodone. And so Trazodone is certainly not a medication a pilot could take every night to help with sleep or depression.
The other serotonin modulators are relatively new to the market. Viibryd came out in 2011 and Trintellix in 2013. Viibryd is available as a generic version, but Trintellix is still only available as the more expensive brand name version. As these medications are newer, cheaper options have been available since their release, so it is rare to ever get to a point that these medications would be approved to be paid for by insurance companies. Because of this, there is not much clinical experience with these medications. So it is hard to recommend them for pilots. Perhaps as the cheaper generic versions of Viibryd and Trintellix become available, more clinical experience with these medications will make prescribers more comfortable with them and insurance companies more likely to pay for their use. But with limited data on their effects in the general population it may be some time until these are considered for approval in pilots.
Another antidepressant that doesn’t really fit in the other categories is Remeron. This is considered an atypical antidepressant. This medication is often used when depression or anxiety symptoms are causing insomnia. As you can see from the chart Remeron is a 4 out of 4 when it comes to causing sleepiness. And it is usually really helpful for getting patients to sleep when they have been struggling with this due to depression or anxiety. Unfortunately, it also tends to cause weight gain as noted by the 4 out of 4 in this column on the chart. So while Remeron may be helpful in depression and anxiety, many patients don’t want to take it due the weight gain. But even without the weight gain, the sedative qualities and 30 hour half-life would mean a pilot would have to wait about 6 days for those 5 half-lives the FAA requires for a sedating medication to be out of your system before flying. So again, not a viable option for a pilot to take every day.
The last category of antidepressants are the tricyclic antidepressants (TCAs). These were the class of antidepressants that were used to treat depression in the ‘60s, ’70s, and ‘80s before the SSRIs came along in the late 20th century. Unfortunately, these medications have poorly tolerated side effect profiles including sexual side effects, weight gain, and sleepiness along with relatively short half-lives. These would mostly likely only be used if most of the SSRIs, SNRIs, and serotonin modulators were unsuccessful in treating someone’s depression. And regardless of the side effects of the TCAs, the level of treatment resistant depression that would require their use would suggest a severe level of depression that was too concerning for flight safety.
As we prepare for touchdown on this series of flights on antidepressants I hope you have found some value in them. These were some of the more technically complex posts I’ve done so far, but I hope I was able to explain them in a way most could follow along. Going into the holidays I think I will back off on the more technical stuff and provide some ways to manage stress many people feel around this time of year. While I didn’t receive much feedback on it, the Upgrade #1 post with the visualization meditation is the most viewed edition of the newsletter, and so it would seem people may be interested in some more mindfulness tracks. So look for some more of these in the coming weeks.
For now I’ll leave you with this…
Seeking Aeromedical Guidance
I hope this summary of antidepressants not approved by the FAA has been helpful. It is essential to remember that every medication has potential side effects, and its effectiveness can vary from person to person. When considering starting an antidepressant as part of your mental health strategy, consulting with an Aviation Medical Examiner (AME) familiar with the FAA’s guidelines is crucial. AMEs can provide guidance on how to navigate the process safely, ensuring that your well-being and aviation career can coexist harmoniously.
I’m certified by the FAA as an AME and as a HIMS Psychiatrist. So I would be happy to consult with you confidentially on any mental health related aeromedical questions. I have looked up other services like this on the internet and they can charge as much as $90 per question. So for my newsletter subscribers and podcast listeners I figure you deserve at least 50% off that. And so, if you have a mental health related aeromedical question you’d like me to address confidentially, just email me at kevinheacockmd@flightshrink.com and for just $45 I’ll address your question.
It can be about any mental health related questions you need help with. Whether that be questions about a mental health condition and how it might affect your medical certificate, how antidepressants might impact your career, or what evaluations the FAA will want if you’re trying to get a special issuance for your mental health condition. Whatever it is, email me at kevinheacockmd@flightshrink.com and for just $45 you’ll get your answer from an FAA certified AME and HIMS Psychiatrist with over 17 years of aeromedical experience.
Support The Flight Shrink:
Stay tuned to The Flight Shrink for more insights into mental well-being and personal development. Your support means so much to me. I love writing this newsletter for you. If you find The Flight Shrink valuable, I invite you to subscribe and share this post with your fellow aviators, friends, family, and colleagues. Your engagement helps us continue this important conversation. Leaving a 5-star review on Apple Podcasts or Spotify can make a big difference too and may even help us get some guests in the future. And now, you can support The Flight Shrink with a one time contribution of any amount on Venmo to username @flightshrink.
Let's soar to new heights while prioritizing our mental health.
I love hearing from readers and listeners, so feel free to Email me at kevinheacockmd@flightshrink.com. Also, you can connect with me on Instagram, X (formally Twitter), Facebook, and Threads with the handle @flightshrink. I also have been more active on LinkedIn recently and you can find me there as Kevin Heacock. And feel free to visit The Flight Shrink substack for archived posts covering a wide range of mental health topics. Until next time...
I'm Dr. Kevin Heacock, The Flight Shrink... Keep on flyin'!